EMBARGOED FOR RELEASE | March 25, 2012
Some scum! Microbe in pond scum enlisted in new cancer test
Note to journalists: Please report that this research was presented at a meeting of the American Chemical Society
A press conference on this topic will be held at 12:30 p.m. Eastern Time, March 25, 2012, in the ACS Press Center, Room 15A, in the San Diego Convention Center. Reporters can attend in person or access live audio and video of the event and ask questions at www.ustream.tv/channel/acslive.
SAN DIEGO, March 25, 2012 — Scientists are enlisting the living, self-propelled microbes found in pond scum — the pea-green surface slicks that form on ponds — in the development of a long-awaited new test to detect the cells that spread cancer through the bloodstream from the original tumor to new sites in the body.
Media Contact
During the meeting, March 23-28, the contacts can be reached at 619-525-6268.
Michael Bernstein
202-872-6042
m_bernstein@acs.org
Michael Woods
202-872-6293
m_woods@acs.org
In a report here today at the 243rd National Meeting & Exposition of the American Chemical Society (ACS), the world’s largest scientific society, they described how the test is intended to not only identify the spreading of cells, but allow lab analysis of those cells so that doctors can decide on the most effective treatment.
Yoshinobu Baba, Ph.D., a renowned scientist who led the research using the pond scum microbe called Euglena, also discussed promising results with new agents that can both produce images of diseased tissue and deliver treatments.
Baba’s team turned to Euglena in an effort to solve the medical problem of detecting the minute number of cancer cells that break off from the original, or primary, tumor site and travel through the bloodstream. Those cells, termed circulating tumor cells (CTCs), enable cancer to spread, or metastasize, and start growing at distant sites in the body. Metastasis is the main reason why cancer can be such a difficult disease to treat. Detecting those cells would raise a red flag so that doctors could treat or more intensively monitor patients. Baba pointed out, however, that the small numbers of CTCs make that goal very difficult.
“In every 20 drops of blood, there are over 5 million white blood cells and 4 billion red blood cells, but there may be only one CTC,” explained Baba, who is with Nagoya University in Japan. “It is very hard to separate such small numbers of CTCs from the huge numbers of blood cells. After separation, we must also get information about the CTCs, such as the DNA sequence. That DNA sequence can provide further confirmation that that cancer has spread, lowering the risk of false alarms and perhaps help with decisions about treatment.”
Baba’s solution is a test that takes place in a lab-on-a-chip, a small device made up of microchambers and channels for the Euglena, which are single-celled organisms with features of both plants and animals. Historians think Euglena are the organisms that Dutch microscope pioneer Anton van Leeuwenhoek saw in 1674 in a sample of pond water. They have chlorophyll to produce food from sunlight, for instance, and also can ingest food. They have a primitive “eye” and a long tail or flagellum that moves like a whip to propel them through the water.
The scientists decided to use Euglena as a natural cargo carrier. Baba’s team attaches an antibody onto the Euglena. That antibody can specifically bind to CTCs. The microbe (with antibody attached) is then placed into a microchamber that contains normal cells and a single CTC, simulating the very low concentration of CTCs that would be in a real cancer patient’s blood sample. The antibody on the microbe binds to the cancer cell. When the researchers shine a light on the microchamber, the Euglena, with CTC in tow, moves to a neighboring microchamber to escape from the light. Afterwards, the CTC could be removed from the microbe and tested further.
They are working on improvements so that the test will reliably detect very small concentrations of CTCs in real blood samples. They plan to couple the microchamber to a so-called nanopore, which can sequence the CTC’s DNA after the separation to positively confirm cancer metastasis.
Baba also is developing “theranostics,” which combine therapy or treatment of disease with diagnostic imaging. One of Baba’s theranostics involves therapeutic stem cells that are combined with imaging agents called “quantum dots,” which are semiconductor crystals that light up when exposed to a special type of light.
“One of the medical doctors in our university hospital injected stem cells into a mouse with liver failure, and the mouse improved,” said Baba. “But he didn’t know how this improvement happened. To determine the mechanism, we made a new type of quantum dot that would be placed inside the stem cells.”
The new quantum dots are biocompatible and are safe for use with living cells, unlike many currently available versions. The quantum dots allowed the researchers to see where the therapeutic stem cells went after they were injected into a mouse.
Baba is now working with medical device companies to commercialize these new tools.
The scientists acknowledged funding from the Japan Society for the Promotion of Science (JSPS) through its Funding Program for World-Leading Innovative R&D on Science and Technology (FIRST Program).
To automatically receive news releases from the American Chemical Society contact newsroom@acs.org.
###
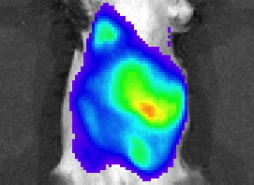
seen in the liver of a living mouse.

